Title: Pneumocystis Choroiditis: A Case Report and Literature Review.
Submitted by: Mariana Vélez Pintado
Institution: Centro Médico ABC
Email: velezpma@gmail.com
Date Submitted: 07/01/2025
History:
A 52-year-old Mexican woman with a recently positive HIV antibody assay and no treatment was evaluated in the clinic. She denied any significant medical history. Her symptoms began in June 2024 with a non-dysenteric diarrhea that continued for approximately 3 months and improved without any therapy.
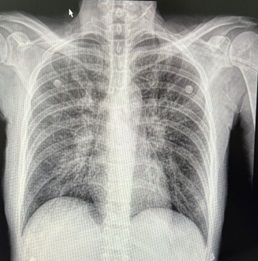
Two weeks before coming to the clinic she complained of a generalized pressure headache that occurred once a week, with an intensity of 8/10, also accompanied by persistent tinnitus. In addition, she also complained of a nonproductive cough with dyspnea on medium exertion and occasional chest pain when breathing for over 1 week. She denied fever or chills. Chest X-ray showed bilateral diffuse infiltrates (Figure 1).
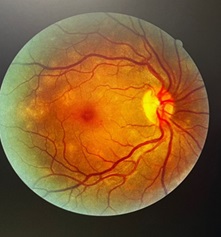
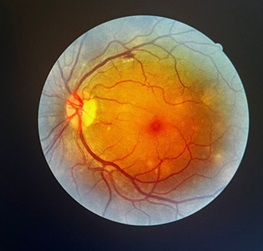
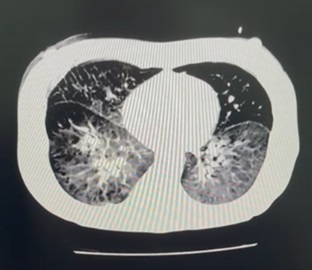
Treatment was started with oral trimethoprim/sulfamethoxazole at 20 mg/kg/day (calculated based on the trimethoprim component) divided every 8 hours while the antiretrovirals were delayed. The patient was sent for ophthalmologic evaluation where Pneumocystis choroiditis was diagnosed (Figures 3 and 4). The patient was contacted for immediate reevaluation. She arrived at the clinic with supplemental oxygen at 5 l/min which was started by a private physician. Her oxygen saturation was 76% off oxygen with some respiratory distress. She was referred to the emergency room where noninvasive mechanical ventilation was started. Thoracic CT scan showed disseminated ground glass infiltrations in both lungs (Figure 4). After 7 days of treatment, she showed clinical improvement and a lower oxygen requirement. HAART was started 48 hrs later. Unfortunately, she had a sudden drop in the oxygen saturation and suffered a cardiorespiratory arrest, return to spontaneous circulation was not achieved and the patient expired.
Physical Examination:
The physical examination during the first medical visit in the clinic, the patient had a blood pressure of 100/70 mmHg, HR 110/min, RR 17/min, O2 Sat 94% on room air and 36.2°C. She had no evident neurological alterations or abnormalities in visual acuity. The oral cavity had white plaques consistent with oropharyngeal candidiasis, and a mobile, nontender, small cervical adenopathy. The lungs had bilateral diffuse rales. Cardiac auscultation was unremarkable. Mild edema was evident in the lower limbs. The rest of the physical examination was within normal limits.
Laboratory Examination:
The patient had an initial HIV viral load of 110,677 copies/mL and a CD4 count of 53 cells/ mm3, taken a week before the first clinical consult.
Question 1: What are probable/possible diagnoses?
Microbiology/Diagnostic Tests Performed:
- Serologies for hepatitis B, hepatitis C, toxoplasma IgM/IgG and syphilis were negative.
- Negative aerobic, fungal, mycobacterial and anaerobic sputum culture. Negative sputum geneXpert, a negative urinary histoplasma antigen, and a negative cryptococcal serum antigen.
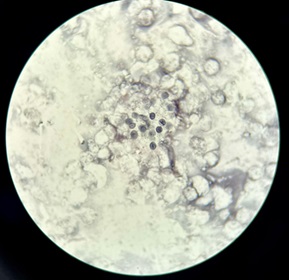
- Toluidine blue O stain in sputum: positive for PJP (Figure 5).
Chest X-ray showed bilateral diffuse infiltrates (Figure 1).
Thoracic CT scan: the lungs presented disseminated ground glass opacities (Figure 4).
The findings of the ophthalmologic examination: Visual acuity was 20/25 for both eyes. There was no evidence of inflammation in the anterior chamber or the vitreous, however multiple round, white-yellow, poorly defined lesions were found. It corresponded to Pneumocystis jirovecii choroiditis (Figures 2 and 3).
Final Diagnosis: Disseminated Pneumocystis jirovecii (pneumonia and choroiditis).
Question 2: What treatment is recommended in the care of this patient?
Treatment: trimethoprim/sulfamethoxazole (first oral then intravenous), oxygen, hydrocortisone, BIC/TAF/FTC
Outcome: Death
Discussion: (500 words)
Pneumocystis choroiditis is an infection caused by Pneumocystis jirovecii, a fungus that mainly affects lungs but can infect other parts of the body such as the eye, spleen, lymph nodes, liver, intestines, bone marrow and heart. This pathogen is found worldwide.This fungus usually affects people living with advanced HIV (less than 200 or less than 14% CD4+), patients using steroids, oncologic patients, and people with solid organ transplants.
When it invades the eye, it usually manifests as choroiditis, it may manifest as visual disturbances or visual loss, but most cases do not present symptoms. This infection is typically diagnosed through imaging and ocular examination. This condition is rare and is a marker of Pneumocystis jirovecii disseminated disease.
This disseminated presentation of the infection was usually found and previously reported in patients who had prophylactic inhaled pentamidine. The patient described in the present clinical case presented with Pneumocystis choroiditis associated with Pneumocystis pneumonia and probable disseminated pneumocystosis, but she did not have previous use of any prophylactic treatment, this presentation was probably associated with long term immunosuppression and fungal infection.
In the pre-HAART era, the frequency of Pneumocystis choroiditis was about 1% in people with less than 200 CD4.
The use of prophylactic inhaled pentamidine was considered a risk factor for dissemination and choroiditis caused by this fungus.
In 1991 a 21-patient cohort with AIDS and Pneumocystis choroiditis was studied, they described choroid round, irregular and yellow to pale yellow lesions. 86% had received inhaled pentamidine, low survival was reported with a range of 2-36 weeks, and few developed visual symptoms.
Most reported cases describe an initial Pneumocystis pneumonia before the diagnosis of Pneumocystis choroiditis or the presence of visual symptoms. In a study published by B E Sha et al, they found a median of 11 CD4 in patients with Pneumocystis choroiditis and reported a mortality of 37.8% associated with this clinical finding.
Gupta et al published a clinical report describing a woman with cotrimoxazole prophylaxis who developed Pneumocystis choroiditis and had good outcomes after treatment. Another case published by K Sabri et al reported retinal detachments in an immunosuppressed non-HIV person caused by Pneumocystis jirovecii. Rugli et al described a case of conjunctival Pneumocystis jirovecii diagnosed by histology that had received 18 months of aerosolized pentamidine prophylaxis. Unger et al published a case of Pneumocystis disseminated infection confirmed with histopathology that reported infiltration of the microorganisms in the arterioles.
Since it is a rare infection presentation there are no studies that suggest how to manage these patients, especially if initial oxygen saturation is normal. Since Pneumocystis choroiditis is a marker of disseminated disease patients should be closely monitored and/or hospitalized for management, there is no sufficient data to recognize this eye infection as a predictor of poor evolution or outcome. Use of steroids should be considered because of the burden of disease but studies are required to determine the benefits. We should consider sending people with advanced HIV to an ophthalmology evaluation in the context of Pneumocystis pneumonia.
Key References:
- Invernizzi, A. (2016). Differential Diagnosis of Infectious Choroiditis. In: Gupta, V., Nguyen, Q., LeHoang, P., Herbort Jr., C. (eds) The Uveitis Atlas. Springer, New Delhi. https://doi.org/10.1007/978-81-322-2506-5_32-1
- Uy HS, Yu-Keh E, Chan PS. Posterior Uveitis. Dev Ophthalmol. 2016;55:163-6. doi: 10.1159/000438968.
- Freeman WR, Gross JG, Labelle J, Oteken K, Katz B, Wiley CA. Pneumocystis carinii choroidopathy. A new clinical entity. Arch Ophthalmol. 1989 Jun;107(6):863-7. doi: 10.1001/archopht.1989.01070010885036.
- Walzer PD, Smulian AG, Miller RF. Pneumocystis species. In: Bennett J, Dolin R, Blaser M, eds. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 8th ed. New York, NY: Saunders; 2015:3016-3030 .
- Siegel M, Masur H, Kovacs J. Pneumocystis jirovecii Pneumonia in Human Immunodeficiency Virus Infection. Semin Respir Crit Care Med. 2016 Apr;37(2):243-56.
- Freeman WR, Gross JG, Labelle J, Oteken K, Katz B, Wiley CA. Pneumocystis carinii choroidopathy. A new clinical entity. Arch Ophthalmol. 1989 Jun;107(6):863-7. doi: 10.1001/archopht.1989.01070010885036.
- Shami MJ, Freeman W, Friedberg D, Siderides E, Listhaus A, Ai E. A multicenter study of Pneumocystis choroidopathy. Am J Ophthalmol. 1991 Jul 15;112(1):15-22. doi: 10.1016/s0002-9394(14)76206-3.
- Gupta A, Hustler A, Herieka E, Matthews BN. Pneumocystis choroiditis. Eye (Lond). 2010 Jan;24(1):178. doi: 10.1038/eye.2009.52.
- Sha BE, Benson CA, Deutsch T, Noskin GA, Murphy RL, Pottage JC Jr, Finn WG, Roth SI, Kessler HA. Pneumocystis carinii choroiditis in patients with AIDS: clinical features, response to therapy, and outcome. J Acquir Immune Defic Syndr (1988). 1992
- Sabri K, Bibby K. Choroiditis and exudative macular detachments in a post transplant leukaemic patient: an unusual presentation of Pneumocystis jiroveci infection. Br J Ophthalmol. 2006 Jan;90(1):118-9. doi: 10.1136/bjo.2005.077479.
- Ruggli GM, Weber R, Messmer EP, Font RL, Moll C, Bernauer W. Pneumocystis carinii infection of the conjunctiva in a patient with acquired immune deficiency syndrome. Ophthalmology. 1997 Nov;104(11):1853-6. doi: 10.1016/s0161-6420(97)30017-7.
- Unger PD, Rosenblum M, Krown SE. Disseminated Pneumocystis carinii infection in a patient with acquired immunodeficiency syndrome. Hum Pathol. 1988 Jan;19(1):113-6. doi: 10.1016/s0046-8177(88)80327-7.
- Rao NA, Zimmerman PL, Boyer D, Biswas J, Causey D, Beniz J, Nichols PW. A clinical, histopathologic, and electron microscopic study of Pneumocystis carinii choroiditis. Am J Ophthalmol. 1989 Mar 15;107(3):218-28. doi: 10.1016/0002-9394(89)90303-6.
- Apostolopoulou A, Fishman JA. The Pathogenesis and Diagnosis of Pneumocystis jiroveci Pneumonia. J Fungi (Basel). 2022 Nov 5;8(11):1167. doi: 10.3390/jof8111167.
- Gupta S, Bebell LM. When should I give corticosteroids to my patient with Pneumocystis pneumonia? Cleve Clin J Med. 2024 Apr 1;91(4):217-219. doi: 10.3949/ccjm.91a.23082.
