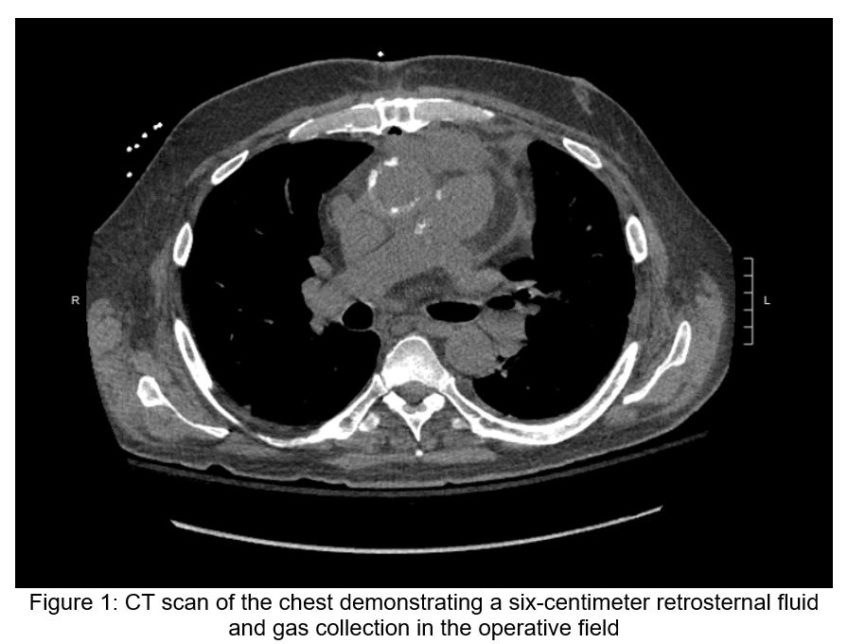
December 2025 Case of the Month
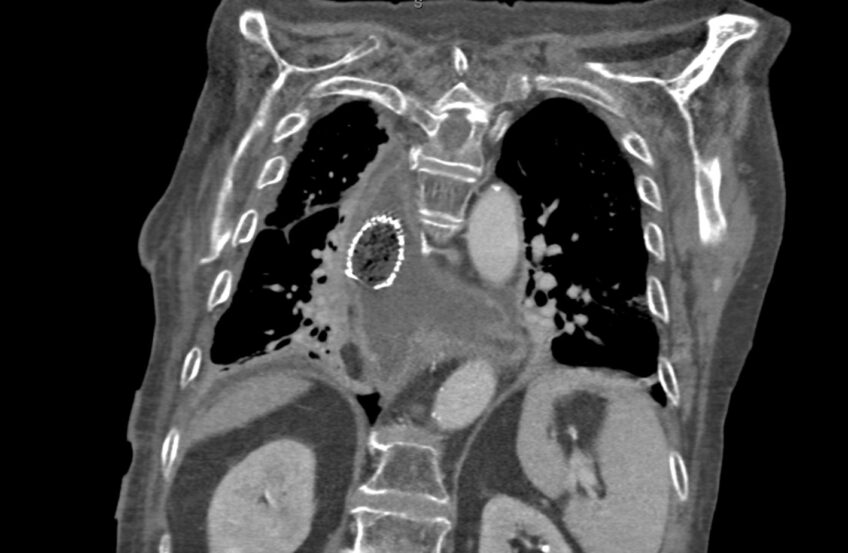
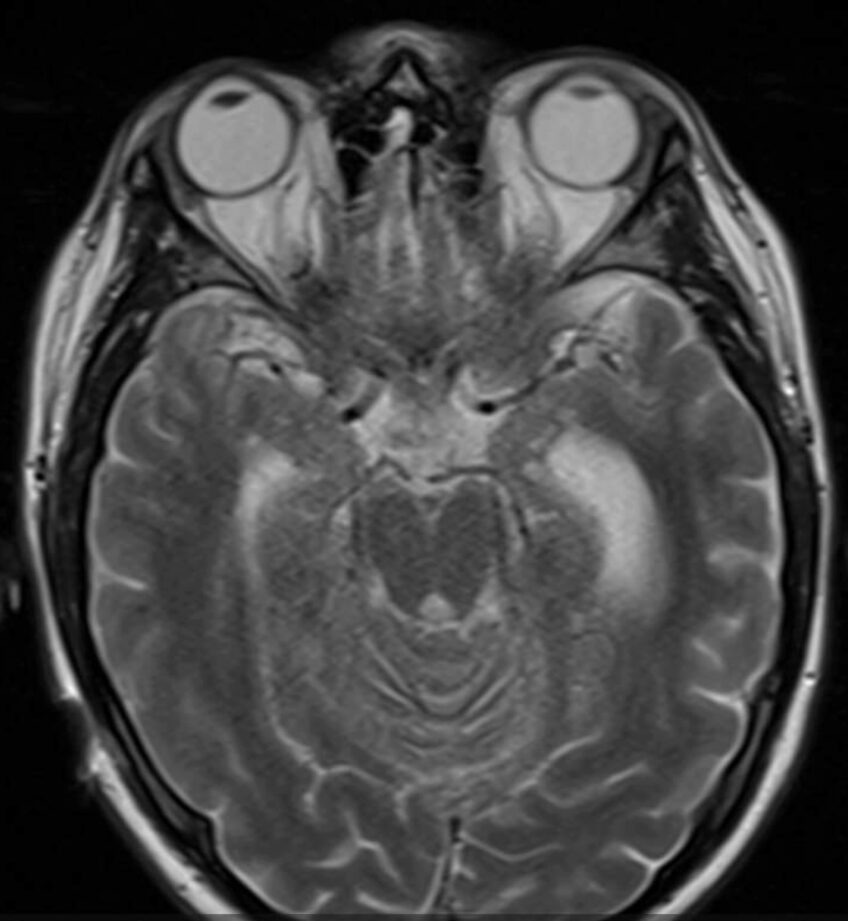
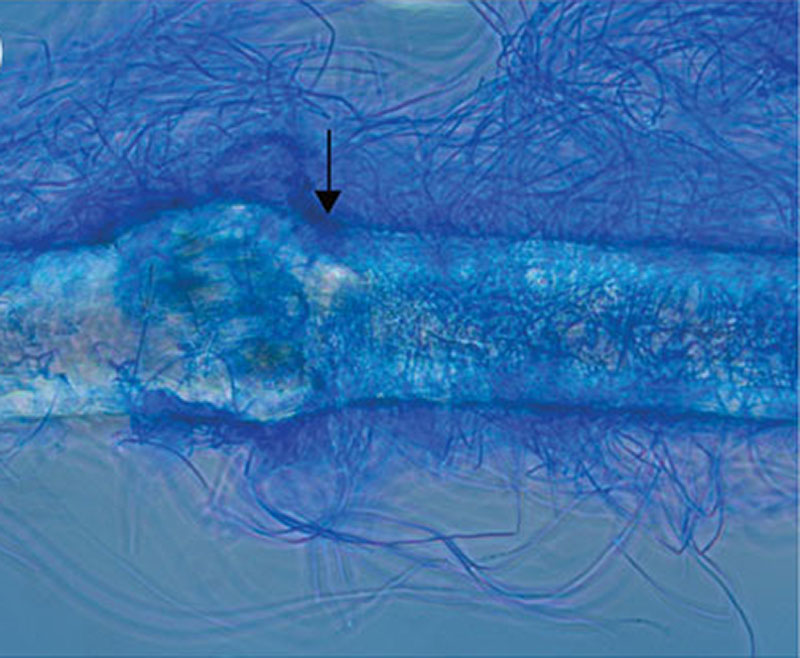
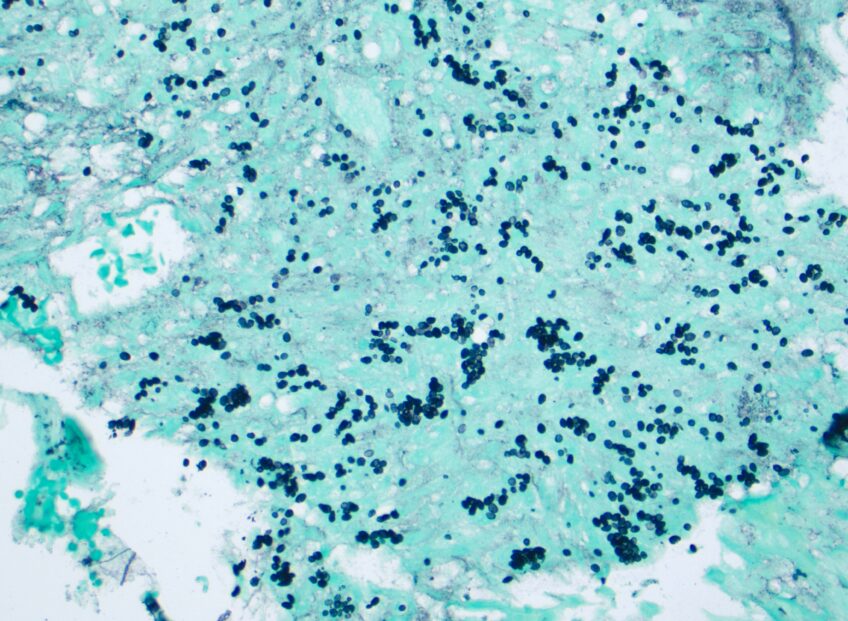
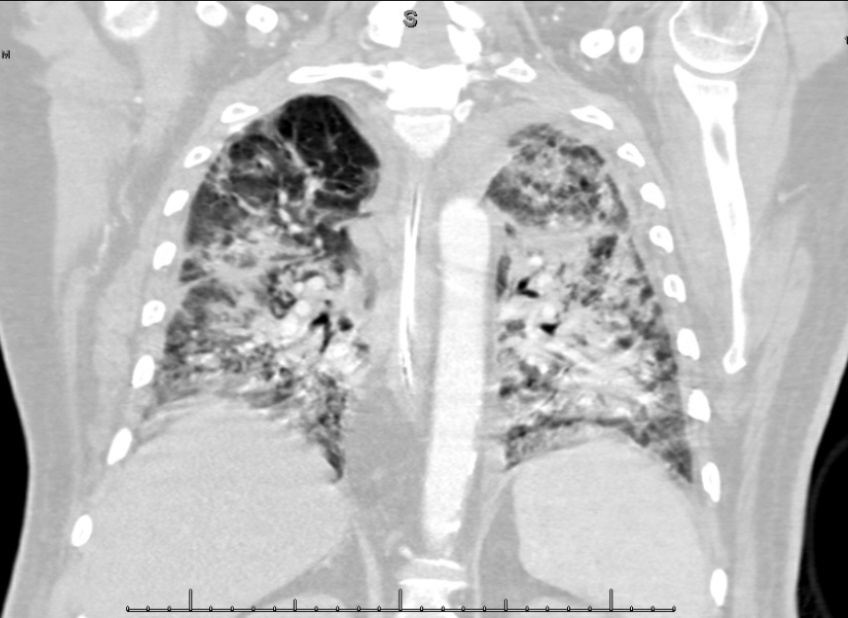
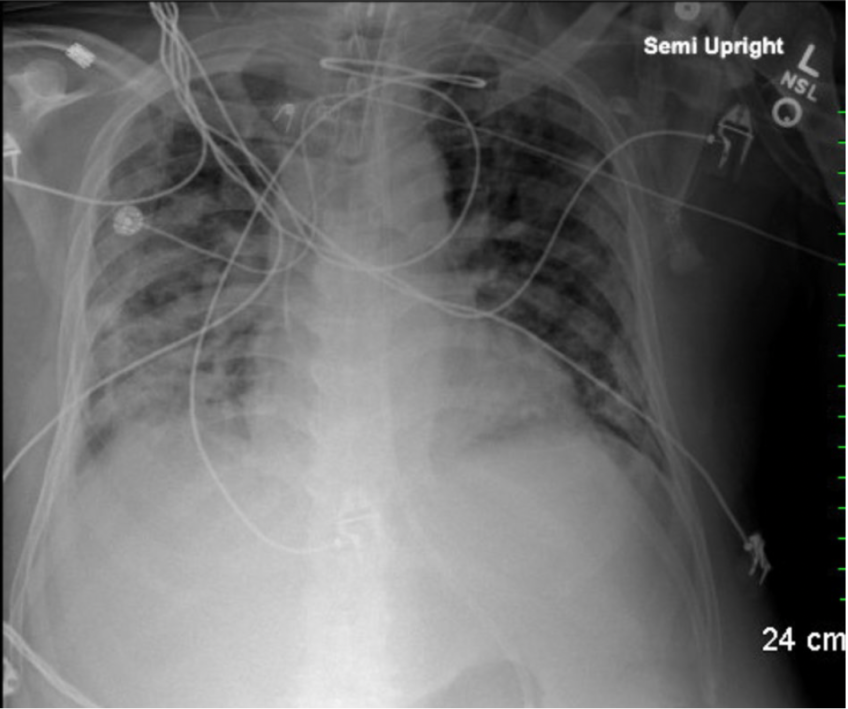
A 35-year-old Filipino woman with an unremarkable past medical history, originally from Seattle, WA and residing in Tucson, Arizona since 2013, developed flu-like symptoms, including cough, fever, chills, night sweats, and malaise in November 2024. She was initially treated with a short course of antibiotics and prednisone at an urgent care clinic, with minimal improvement.