Title: Disseminated Coccidioidomycosis in a Patient Receiving Ruxolitinib
Submitted by: Karolina Perez, Leah Friedman, Mehraneh Mohseni Zadeh Harouzi, Rachel Wu, Fariba Donovan
Institution: Valley Fever Center for Excellence, Banner University Medical Center-Tucson, University of Arizona, College of Medicine-Tucson, Arizona
Email: kperez1813@arizona.edu
Date Submitted: 5/31/25
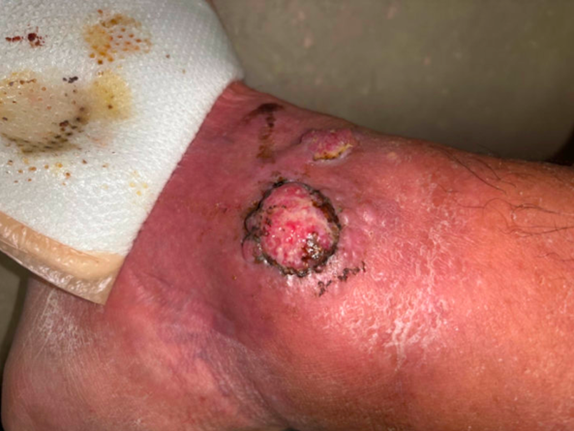
History: The patient is a 74-year-old Caucasian male from Colorado who is a part time resident of Arizona since 2015. He presented to the outpatient infectious disease clinic with a lesion on the lateral aspect of the right ankle (Figure 1) that had been slowly enlarging in size over the past two years. The lesion extended proximally towards the lateral knee, medial thigh (Figure 2), and into the right groin area with associated purulence and drainage. His past medical history includes hypothyroidism, hypertension, resected prostate cancer, and polycythemia vera treated with ruxolitinib since 2017.
Pertinent Physical Examination:
Musculoskeletal: Right ankle has chronic excoriating 1.5 cm lesion with purulent/serosanguineous discharge with surrounding edema and associated limitation in range of motion of right ankle. (Photo 1). There was warmth, pain, and discomfort during examination.
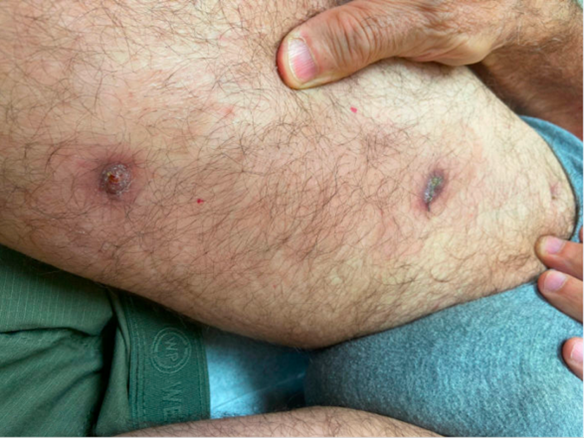
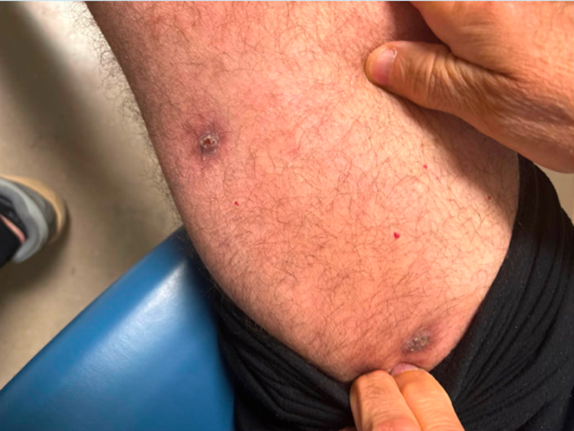
Skin: Extensive ascending lymphangitis along the lateral aspect of the right ankle, knee upward to medial aspect of right thigh extending to right groin area with purulent discharge (Photo 2 and 3).
Laboratory Examination: Complete blood count (CBC) demonstrated a white blood cell count of 10.1 K/μL, hemoglobin of 11.1 g/dL, mean corpuscular volume (MCV) of 82 fL, and platelet count of 434 K/μL. Absolute neutrophil count was 8.08 K/μL and absolute lymphocyte count was 0.5 K/μL.
Comprehensive metabolic panel (CMP) revealed a creatinine level of 1.07 mg/dL and blood urea nitrogen (BUN) of 31 mg/dL. Liver enzymes were within normal limits with an AST of 29 U/L and ALT of 17 U/L.
Coccidiomycoidal Complement Fixation Titer 1:64.
Question 1: What are probable/possible diagnoses?
Microbiology/Diagnostic Tests Performed: Biopsy, culture, and MRI of femur and tibia
Final Diagnosis: Disseminated Coccidiomycosis with right ankle septic arthritis and associated ascending lymphangitis along the right leg and right thigh.
MRI findings: Heterogenous bone marrow signal within the pelvis and proximal left femur without focal enhancement. There is a multiloculated rim-enhancing fluid collection within the medial thigh subcutaneous tissues measuring 3.8 x 2.3 x 6.8 cm which abuts a thickened superficial fascia of the medial compartment of the thigh, consistent with abscess and superficial fasciitis. 22 x 10 mm subdermal lesion over the lateral malleolus.
Biopsy of right ankle: Coccidioidal spherules
Culture was positive for Coccidioides species and scant growth of Corynebacterium, Staphylococcus epidermidis, and Finegoldia magna.
Question 2: What treatment is recommended in the care of this patient?
Treatment:
- Initial intervention was surgical debridement of the affected sites including incision and drainage (I&D) of the right ankle and right thigh with amphotericin deoxycholate bead placement. The patient required further surgical debridement and exchange of antifungal beads.
- While hospitalized, patient received liposomal amphotericin B as well as short course antibacterial treatment for superimposed infection.
- He was discharged on fluconazole 800 mg. Other azoles were contraindicated considering need for continuation of ruxolitinib.
- A 3-week course of doxycycline 100 mg twice daily and amoxicillin-clavulanate 875 mg twice daily for superimposed bacterial infection.
- Patient is stable on current management with fluconazole 800 mg daily. He will likely require lifelong fluconazole therapy to prevent future reoccurrence of Valley fever.
Outcome:
- Patient clinically stable on fluconazole 800 mg following 3-week hospitalization
- Continues routine follow up with orthopedics infectious disease
- Continues regular wound care
- Recently restarted on low dose Jakafi with routine hematology follow up
- Plans to return to Colorado in summer
Discussion: (500 words):
The management of coccidioidomycosis in patients receiving immunosuppressive therapies, such as Janus kinase (JAK) inhibitors (ruxolitinib, Jakafi®) presents complex clinical challenges. Treatment decisions must account for potential drug-drug interactions and the risk of toxicities associated with both immunomodulatory agents and azole antifungal treatments. In immunocompromised individuals living in coccidioidomycosis-endemic regions, early diagnosis and serological testing is essential to reduce the risk of disease progression and to guide the safe and effective use of immunosuppressive treatments.
The patient developed pneumonia and shortness of breath in 2022 with minimal improvement after antibiotics. Laboratory workup was inconclusive, and he was empirically started on fluconazole for presumed pulmonary coccidioidomycosis. His respiratory symptoms of cough and shortness of breath resolved and therefore fluconazole was discontinued. It is important to consider that the patient is immunocompromised and has been receiving ruxolitinib for polycythemia vera since 2017.
In 2023, the patient presented to dermatology after noticing a lesion on the right ankle. The lesion was biopsied and found to be negative for malignancy. Over the next several months, he noted extension of the wound to the lateral knee, medial thigh, and into the right groin.
When he began taking fluconazole for presume coccidiomycosis infection, his dose of Jakafi was adjusted although the exact changes were unclear from chart review. The patient had evidence of disseminate coccidioidomycosis that presented almost a year after patient stopped fluconazole after symptoms resolved for pulmonary coccidioidomycosis.
This case highlights a rare presentation of disseminated coccidioidomycosis involving subcutaneous and soft tissue infection complicated by polymicrobial superinfection in an immunocompromised host on JAK inhibitor therapy. The patient had been on ruxolitinib with good symptom control for polycythemia vera for several years. Upon initiating fluconazole for presumed pulmonary coccidioidomycosis, his ruxolitinib dose was adjusted although the specific changes were unclear from chart review. Nearly a year after discontinuing fluconazole following resolution of pulmonary coccidioidomycosis symptoms, the patient developed disseminated disease.
Evaluation of the host immunity is critical in understanding the risk of serious coccidiomycosis infection. This risk is particularly pronounced, increasing by up to 150-fold in immunosuppressed individuals. Biologic response modifiers such as JAK-inhibitors are immunomodulary medications used to treat autoimmune disease by downregulating the host immune responses. Our patient’s chronic use of ruxolitinib likely contributed to impaired cellular immunity, increasing the risk of Coccidiodal dissemination. Management was further complicated by significant drug-drug interactions between ruxolitinib and azole antifungals, limiting antifungal options and requiring careful monitoring for adverse events. Early tissue biopsy and fungal culture were essential for establishing the diagnosis. With the unusual presentation of disseminated coccidioidomycosis, healthcare provider awareness and education is essential for clinical suspicion of patients receiving immunosuppressive therapy residing in endemic areas.
Key References:
- Donovan FM, Ramadan FA, Lim JR, Buchfuhrer JE, Khan RN, DeQuillfeldt NP, Davis NM, Kaveti A, De Shadarevian M, Bedrick EJ, Galgiani JN. Contribution of Biologic Response Modifiers to the Risk of Coccidioidomycosis Severity. Open Forum Infect Dis. 2022 Jan 27;9(3):ofac032. doi: 10.1093/ofid/ofac032. PMID: 35169593; PMCID: PMC8833864.
- Cohen IM, Galgiani JN, Potter D, Ogden DA. Coccidioidomycosis in renal replacement therapy. Arch Intern Med. 1982 Mar;142(3):489-94. PMID: 7039544.
- Zou A M, Eze B, D’Souza A, et al. (April 04, 2025) Pulmonary Coccidioidomycosis in a Ruxolitinib-Treated Polycythemia Vera Patient: A Case Study and Literature Review. Cureus 17(4): e81725. doi:10.7759/cureus.81725
- Yael Kusne, Kathryn E Kimes, Fionna F Feller, Roberto Patron, Juan Gea Banacloche, Janis E Blair, Holenarasipur R Vikram, Neil M Ampel, Coccidioidomycosis in Patients Treated With Ruxolitinib, Open Forum Infectious Diseases, Volume 7, Issue 6, June 2020, ofaa167, https://doi.org/10.1093/ofid/ofaa167
