AML with persistent rash
History:
23 yo woman with relapsed AML was recently admitted for re-induction chemotherapy. She became profoundly neutropenic and was managed with empiric antibacterial and antifungal therapy with micafungin. Despite persistent neutropenia, she remained stable afebrile on most days. On day 35 days following admission, she developed worsening fever and her regimen was changed from vancomycin, zosyn, and micafungin to empiric treatment with cefepime, daptomycin, and voriconazole. On Day 36, she developed worsening fever and a progressive palpable, painless, erythematous rash with lesions ranging from 1-2 cms. She remained febrile the on Day 37, with the development of more skin lesions, some with evolving necrotic centers.
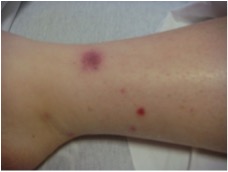
Figure 1 – Right Lower Leg
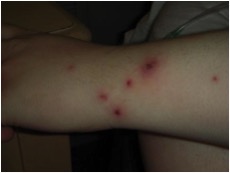
Figure 2 – Left hand/wrist
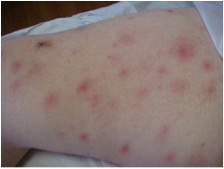
Figure 3 – Left upper leg
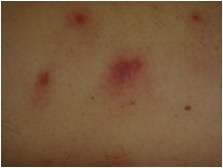
Figure 4 – Left upper leg lesions
Empiric L-AMB 5 mg/kg is added to the regimen. Additional blood cultures and a skin biopsy were performed.
Micro: Blood cultures, results pending
Pathology: Skin biopsy, culture results pending
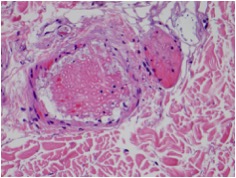
Figure 5 – Biopsy histopathology (H and E stain)
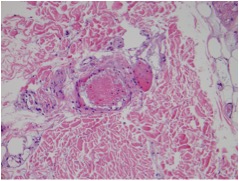
Figure 6 – Biopsy histopathology (H and E stain)
Imaging: none
Hospital course: The patient tolerated L-AMB 5 mg/kg/d and voriconazole 4 mg/kg q12 hours, repeat BC were negative. Pt remained febrile over the next 5 days, gradually worsening with progression of skin lesions. Despite maximum support, she expired day 42 with persistent fever and neutropenia
Diagnosis: Disseminated fusariosis
FUNGAL RESULTS:
All blood cultures and skin biopsy cultures became positive for Fusarium solani.
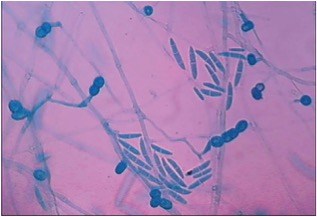
Figure 7 – Fusarium solani (Image credit: M. Kudar (2013)
Question: What treatment is recommended in the care of this patient?
- There are no generally accepted guidelines for treatment of fusariosis
- There is no consistently active AF agent vs Fusarium Limited data suggest voriconazole is effective in approx 50% of pts.
- There are less data pertaining to treatment with posaconazole, isavuconazole, and combination therapy with an expanded spectrum azole plus amphotericin B.
Discussion:
- Disseminated fusariosis is the 2nd or 3rd most common mold infection among patients with advanced hematological malignancies, following aspergillosis and +/-mucormycosis
- Fusariosis is particularly common among patients with relapsed disease and with profound and prolonged neutropenia.
- Skin lesions, especially of the extremities, some with evolving necrotic centers are characteristic.
- Unlike invasive aspergillosis, where blood cultures are rarely positive, blood cultures are positive in up to 60% of patients with disseminated fusariosis.
- Neutrophil recovery is critical to successful treatment and survival.
- There are no data to suggest a correlation between antifungal MIC and outcome.
Key References:
- Improvement in the outcome of invasive fusariosis in the last decade. Nucci M, Marr KA, Vehreschild MJ, et al. Clin Microbiol Infect. 2014;20:580-5
- Nucci F, Nouér SA, Capone D, Anaissie E, Nucci M. Semin Respir Crit Care Med 2015;36(5):706-14
- Treatment and outcomes of invasive fusariosis: review of 65 cases from the PATH Alliance(®) registry. Horn DL, Freifeld AG, Schuster MG, Azie NE, Franks B, Kauffman CA. Mycoses. 2014;57:652-8

Thank you for presenting this case. In difficult situations such as this, I am wondering if you, or any of the readers have experience using immune stimulants such as the checkpoint inhibitors to try to control the infection?