Overview
Within the four overlapping forms of invasive candidiasis, there is a distinct clinical picture that has been given a variety of names: Chronic Disseminated Candidiasis (CDC), Hepatosplenic Candidiasis, Hepatic Candidiasis and Granulomatous Hepatitis.
As proposed by Bodey, we will generally use the term hepatosplenic candidiasis [271]. However, the other terms are equally valid.
At least in theory, a separation should be made between this entity and liver involvement in cases of acute disseminated candidiasis [273]. Cases of acute disseminated disease can certainly become chronic [2233].
Epidemiology
The precise incidence of Hepatosplenic Candidiasis is unknown. Difficulties in diagnosing this entity make any attempt to estimate its actual incidence inaccurate. However, in a study of 562 adult patients with leukemia, an incidence of ~ 7% was found [106]. In this center a fivefold increase in the incidence of this condition was reported for the period 1980 to 1993. A report of fatal cases in bone marrow recipients for the period 1980-1986 found an increase from 2 to 20% among the autopsies of patients who died with fungal liver involvement [1970].
Risk Factors
Interestingly this is a condition that affects almost exclusively patients undergoing remission induction chemotherapy or bone marrow transplantation for acute leukemia [988, 1331, 1970, 2233]. It has been reported that patients with acute lymphocytic leukemia have a higher incidence than those with acute myeloid leukemia [106]. Occasionally, patients with other types of immunosuppression (e.g., aplastic anemia, lymphoma, sarcoma) will develop hepatosplenic candidiasis.
Another remarkable aspect of this condition is that it manifests only on recovery from prolonged periods of neutropenia [988]. It seems that an adequate inflammatory response is necessary to produce the classic clinical picture and thus that recovery from neutropenia is crucial for the development of granulomas in the affected organs [2233].
Hepatosplenic Candidiasis and Candida species
In cases of hepatosplenic candidiasis, microbiological confirmation is even more difficult than for candidemia. Nevertheless, the available data suggest that C. albicans is the leading cause. The usual pathogenic non-albicans species can also cause hepatosplenic candidiasis [106, 2233].
As with other forms of invasive candidiasis, fever is the most consistent clinical sign. In this disease, elevated temperatures can persist for several months [988].
The other near constant finding is one of a group of abdominal symptoms. Right upper quadrant tenderness, hepatomegaly, abdominal distension, nausea, vomiting and diarrhea occur with variable frequency. Left upper quadrant tenderness has also been described.
For physicians dealing with bone marrow transplant recipients, two challenging differential diagnoses include those non-infectious liver conditions that commonly affect this population [1970]. They are veno-occlusive disease of the liver and graft-versus-host disease (GVHD).
To establish the diagnosis of hepatosplenic candidiasis physicians should be persevering and diligent. None of the following diagnostic tools is either pathognomonic or highly sensitive.
Hematologic & Biochemical Findings
- Liver Function Tests. One of the most consistent biochemical findings in hepatosplenic candidiasis is a marked elevation on serum alkaline phosphatase [988]. Other liver function tests like bilirubin, aspartate aminotransferase (serum glutamic oxalacetic transaminase), and gamma glutamyl transferase can also show mild to moderate levels of elevation.
- White Blood Count. Another commonly reported finding among patients with CDC is rebound leukocytosis [2236].
Unfortunately, these laboratory changes are very similar to those found in cases of GVHD and sepsis-related cholestatic liver disease, thus confusing the diagnosis [1970].
Microbiology Data
- Blood cultures are nearly always negative even in the febrile neutropenic phase that proceeds the florid clinical presentation of hepatosplenic candidiasis [988, 2225]. Colonization of the gastrointestinal tract is documented in the majority of cases [988, 1970], but this is of little diagnostic value.
- Culturing Candida from liver biopsies is also difficult. The small size of the specimen and previous treatment with antifungal agents are possible explanations for this finding [988, 2233].
Histopathology
The only conclusive diagnostic tool for this entity, is a histopathologic demonstration of fungal elements in the liver consistent with Candida. Macroscopically the liver and spleen are covered with yellowish nodules from 1 to 2 mm and a well-defined granulomatous lesion with characteristic budding yeasts with or without pseudohyphae is the expected finding. However, liver biopsies do not always render the best results because it is only in the very center of the lesion where fungal elements are found [2233]. Indeed, percutaneous biopsies, even when guided with imaging studies do not always provide good material.
Exploratory laparoscopy has a better yield [988]. Laparoscopy-guided liver biopsy has been also proposed and it has been said that the best yield is obtained when performed soon after recovery from neutropenia [107]. It is important to distinguish the findings of liver involvement in cases of Acute Disseminated Candidiasis from those related to the unique clinical syndrome of Hepatosplenic Candidiasis. In the former, abscess formation is seen, and (if the patient is neutropenic) coagulation and hemorrhagic necrosis will be found. Conversely, in cases of Hepatosplenic Candidiasis, as mentioned above, granuloma formation (not abscess) is characteristic [273].
The absence of organisms in a liver sample showing granulomas does not rule out the disease, particularly when the patient has already received antifungal treatment [2233].
To confirm a clinical suspicion of Chronic Disseminated Candidiasis it is recommended to perform enhanced and non-enhanced computed tomography (CT) as well as liver ultrasound (US) [1728]. The reason being that even when lesions not seen at US are often seen at CT, the opposite is also true. Expected findings are as follows:
- Ultrasound. By ultrasound, the lesions may have a uniformly decreased attenuation or show a central high attenuation dot inside that has been called “wheels within wheels” or “bulls-eye” appearance. [1728, 2099].
|
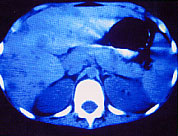 |
- Radionuclide Scans. Radionuclide scans (e.g., 99Tnc, 67Ga ) can show hepatosplenomegaly, diffuse non-homogenous patterns of uptake, but all these findings are very nonspecific [2233].
- Magnetic Resonance Imaging (MRI). By magnetic resonance imaging, nonspecific lesions with relatively low signal intensity of the T1-weighted images and high signal intensity on the T2-weighted images have been described, but the experience with MRI is still limited [1591]. Despite this, it has been suggested that MRI is superior to CT and ultrasound to make the diagnosis [108, 2006]. Authors reporting this advantage, recommend “STIR” imaging as the MR technique of choice at 1.0 T [1288].
It is important to notice that radiologic resolution of these findings does not parallel the clinical response. Some patients may continue having multiple defects on enhanced scans or develop calcified lesions [2098, 2099]. However, the lesions should become stable on serial scans.
Therapies
A high fatality rate has characterized the picture of Hepatosplenic Candidiasis. Even after protracted courses of Amphotericin B with or without 5-fluorocytosine, mortality was initially reported in the range 40-50% [2225]. The introduction of azoles, first ketoconazole and later fluconazole dramatically changed the poor prognosis of patients affected with this entity.
Ketoconazole has the disadvantage of causing liver toxicity and fluconazole has been more extensively studied [61, 1165]. For example, Anaissie et al. reported an 88% success rate with fluconazole among 16 patients who had either failed or became intolerant to Amphotericin B.
Another approach with good results has been the use of the new formulations of lipid-associated preparations of amphotericin B [1365, 2005, 2006]. A theoretical advantage of these formulations of Amphotericin B is the high hepatic concentrations that they produce [535]. Nevertheless, none of these drugs has been studied in a randomized fashion.
The use of interferon-gamma and GM-CSF has also been explored with satisfactory response [1840]. However, these data are anecdotal and randomized studies are required before this strategy reaches the level of a standard recommendation.
A specific length of therapy cannot be recommended. Instead, therapy should continue until complete resolution of symptoms and laboratory abnormalities, as well as imaging study abnormalities (either CT or MRI). In some cases, the imaging studies will convert to calcification and this is considered an acceptable endpoint.
For patients with acute leukemia and CDC, in whom subsequent cycles of chemotherapy are required, stabilization of the infection before continuation of cytotoxic therapy is suggested [2354]. However, the infection need not be cured. Rather, the patient need only show some evidence of improvement. Antifungal therapy should be continued without cessation during the course of chemotherapy.
