Manufacturer’s Prescribing Information
Trade & Generic Names & General Features
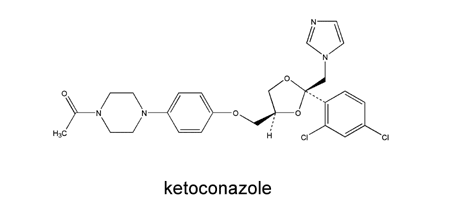
Ketoconazole is an imidazole antifungal agent. As with other imidazoles, it has five-membered ring structures containing two nitrogen atoms. It is marketed as Nizoral™ by Janssen Pharmaceutica ((E):http://us.janssen.com/(E):). Ketoconazole has oral tablet, cream and dandruff shampoo formulations. The oral formulation is available in USA since 1981. Ketoconazole is the only member of the imidazole class that is currently used for treatment of systemic infections.
Ketoconazole is a highly lipophilic compound. This property leads to high concentrations of ketoconazole in fatty tissues and purulent exudates. Expectedly, the distribution of ketoconazole into cerebrospinal fluid is poor even in the presence of inflammation. Its oral absorption and solubility is optimal at acidic gastric pH [2092, 2288].
While ketoconazole was more widely used before the development of newer, less toxic, and more effective triazole compounds, fluconazole and itraconazole, its use has now been limited. It now appears as an alternative drug for specific indications.
Mechanism(s) of Action
As with all azole antifungal agents, ketoconazole works principally by inhibition of cytochrome P450 14a-demethylase (P45014DM). This enzyme is in the sterol biosynthesis pathway that leads from lanosterol to ergosterol [1394]. The affinity of ketoconazole for fungal cell membranes is less compared to that of fluconazole an itraconazole. Ketoconazole has thus more potential to effect mammalian cell membranes and induce toxicity [467].
Susceptibility Patterns
Ketoconazole is active against Candida spp., and Cryptococcus neoformans. However, its activity is limited compared to that of fluconazole and itraconazole [2142]. Furthermore, due to its limited penetration to cerebrospinal fluid, it is clinically ineffective in meningeal cryptococcosis. Its activity against the dimorphic moulds, Histoplasma capsulatum, Blastomyces dermatitidis, Coccidioides immitis, Sporothrix schenckii, Paracoccidioides brasiliensis, and Penicillium marneffei is favorable. However, fluconazole and itraconazole are at least as effective as ketoconazole against these fungi and are safer. Thus, ketoconazole remains as an alternative second-line drug for treatment of infections due to dimorphic fungi. Ketoconazole is not recommended for treatment of meningeal infections due to Histoplasma capsulatum, Blastomyces dermatitidis, and Coccidioides immitis due to its limited penetration to cerebrospinal fluid [467].
Ketoconazole is also active against Pseudallescheria boydii and is a good alternative for treatment of pseudallescheriasis [2092]. It is also effective in pityriasis versicolor [548].
Ketoconazole has practically no activity against Aspergillus spp., Fusarium spp., and zygomycetes order of fungi [467].
For ketoconazole MICs obtained for various types of fungi, see susceptibility patterns and the N/A(L):susceptibility database.
Usual Doses
Oral ketoconazole is used at a dose of 200 to 400 mg/day in treatment of oral and chronic mucocutaneous candidiasis. The recommended dose is 400 mg/day in endemic mycoses due to dimorphic fungi in nonimmunosuppressed hosts [1624]. The dose can be increased to 600-800 mg/day in patients not responding to regular doses. However, high doses carry the risk of high incidence of toxicity [798].
Ketoconazole administered at a single dose of 400 mg/day is effective in treatment of pityriasis versicolor. The single dose therapy can be repeated once every month since recurrence is common with this infection [548].
Side-Effects
The major drawbacks of ketoconazole therapy are from the occasionally seen adverse reactions. It may induce anorexia, nausea and vomiting [467, 598]. Increase in transaminase levels and hepatoxicity may occur [1332, 2369]. Ketoconazole may decrease testosterone and cortisol levels, resulting in gynecomastia and oligospermia in men and menstrual irregularities in women [1663, 2237].
The effects of ketoconazole on functions of the thyroid gland have also been investigated. There have been a number of reports suggesting that (E):ketoconazole may have antithyroid function via impairment of thyroglobin iodination and iodothyrosine coupling. In vitro, ketoconazole has been found to form a complex with iodine and inhibit lactoperoxidase. In vivo experiments in rats have shown that the weight of thyroid gland increases in rats treated with ketoconazole [466]. In another study designed to investigate the influence of ketoconazole on the basal and TSH-stimulated iodide uptake in the rat thyroid cells, concentration-based variations were observed. Ketoconazole appeared to increase the basal iodide uptake slightly at lower concentrations, while it sharply decreased the uptake below the basal levels at higher concentrations. Under TSH stimulation, the inhibitory effect of the drug were observed even at low concentrations [1220]. In contrast to these animal data, studies carried on in a limited number of euthyroid, healthy individuals, hypothyroid patients, and patients with thyrotoxicosis failed to provide any data suggesting a potential inhibitory effect of ketoconazole on thyroid functions [536, 537]. These data suggest that possible antithyroid effect of ketoconazole demands further investigation and close follow-up.
Routes
Ketoconazole has oral tablet, cream and dandruff shampoo formulations.
Current Status
Although an effective compound, ketoconazole has become a second-line drug due to the ready availibility of the somewhat safer agents, itraconazole and fluconazole.
Interestingly, administration of ketoconazole has successfully decreased the serum ionized calcium and 1,25-dihydroxyvitamin D levels in two patients with tuberculosis-associated hypercalcemia [1999]. Also, ketoconazole has provided biochemical and hormonal improvement in patients with paraneoplastic Cushing’s syndrome secondary to ectopic adrenocorticotropin (ACTH) production by malignant neoplasms [2446].
